While a normal healthy cornea has a round shape, a cornea with Keratoconus1 juts out, producing a cone shape instead. The conical shape impairs vision, as it deflects light as it enters the eye on its way to the retina, which uses light to send perception to the brain. The condition affects the eye’s cornea, the outer covering of the iris, pupil and the anterior chamber fluid. Our trained eye doctors help many Orange County residents each year to properly diagnose and treat Keratoconus.
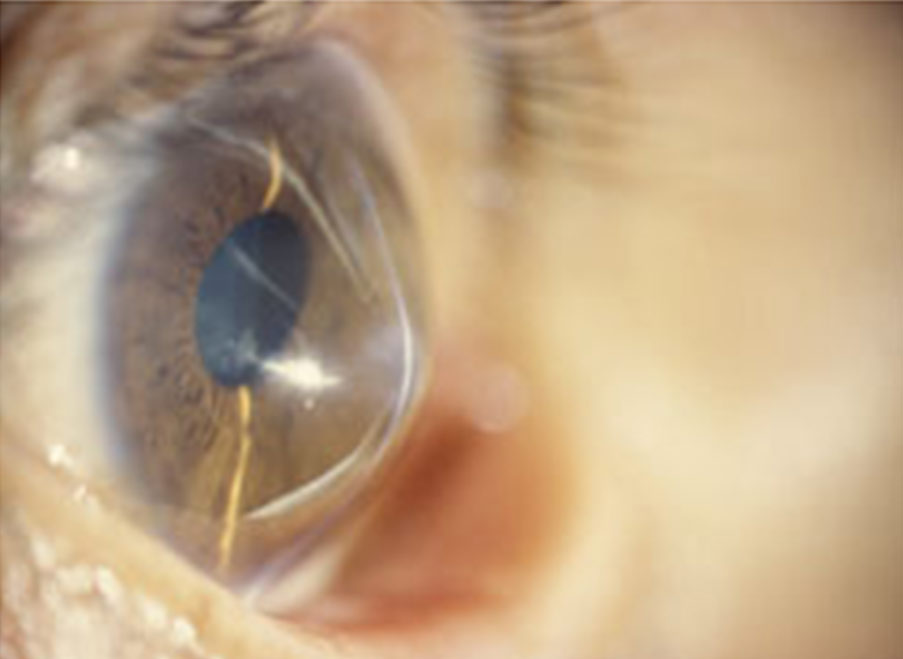
The cornea's shape can be reshaped over time to a weakness in its structure. Although the exact cause of this disease is unknown, recent research links it to an enzyme imbalance, or oxidative stress taking place in the cornea. This weakens the cornea, making it vulnerable to damage from free radicals – harmful compounds left over from cell metabolism. A healthy cornea has its collagen, the fibrous network of proteins, intact, allowing the cornea to remain in place. When the collagen is weakened, the cornea can no longer stay in place and begins to move forward, resulting in a cone shape.
While there are other theories floating around as to what causes Keratoconus that have yet to be proved, genetics remain a predominant factor. Often, people who develop this disease often do so because someone in their family has had it. Keep in mind that chances are small – there is a less than 10% chance that a blood relative of a patient with Keratoconus will develop this condition.
Keratoconus begins in the teenage years or up to the thirties. Distorted vision will ensue as the cornea progresses into a cone shape. Below are the most common symptoms and signs of Keratoconus2. However, many of these symptoms are also present in other eye conditions, so it is best to come in and be diagnosed by one of our eye doctors rather than try to self-diagnose.
Keratoconus can be diagnosed by our eye doctors using the slit-lamp technique. The doctor will search your cornea for thinning areas, an iron-colored ring encircling the cornea (the Fleischer's Ring) and scarring at the outermost part of the cone. It is also important to measure the curvature of the cornea to determine whether it obtained a cone shape. The curvature is measured via Keratometry, which involves an instrument shining light patterns onto the cornea. The shape of the reflection of the pattern shows how the eye is curved. Corneal topography is also used, in which a computer creates three-dimensional "maps" of the cornea.
While Keratoconus is still in its early stages, it can be treated with eyeglasses or rigid gas permeable contact lenses (silicone-based). As the disease worsens, the cornea becomes weakened to a degree that makes it resistant to vision correction from eyeglasses and RGP contacts. Advanced treatment options include:
Cornea Collagen Crosslinking (CXL)3 surgery is an experimental option that can be helpful in preventing progression by way of strengthening corneal tissue.
Intacs4 are inserts surgically implanted into the cornea, placed under the surface of the cornea to reshape the cone form and provide patients with better vision.
Cornea transplant5 may be suggested when all other remedies fail. A donor cornea is transplanted into the eye after the patient's cornea is removed.
References
1 What Is Keratoconus? Available: https://www.aao.org/eye-health/diseases/what-is-keratoconus
2 Keratoconus. Available: https://www.mayoclinic.org/diseases-conditions/keratoconus/symptoms-causes/syc-20351352
3 Corneal Collagen Cross-Linking. Available: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2880370/
4 Your Eyes, Keratoconus, and Intacs. Available: https://www.webmd.com/eye-health/eye-health-intacs
5 Cornea Transplant. Available: https://my.clevelandclinic.org/health/treatments/17714-cornea-transplant
Great experience! When I called to make an appointment, I was able to be seen within a few days. The receptionist was very pleasant and professional. I liked the convenience of being able to print the new patient forms and complete them at home. The in-office wait time was reasonable. Super helpful, professional and pleasant staff. Dr. Jwo is very knowledgeable. He took the time to review my history, asked questions and offered recommendations. He also asked if I was comfortable with the recommendations and whether I had additional questions. I didn't feel rushed, which was very much appreciated. Beach Eye is excellent and Dr. Jwo is an excellent provider.

Medically Reviewed by
Samir Shah, MD
Samir Shah, MD, MS, FACS, is a board-certified ophthalmologist specializing in custom laser cataract surgery and refractive lens exchange. A Johns Hopkins fellow and UCLA alumnus, he is nationally recognized as an expert in refractive cataract surgery. Recently, he was named the Top Doctor 2026 by the Orange County Medical Association and Orange Coast Magazine.