A blocked tear duct occurs when the tear drainage system becomes partially or completely obstructed. While blocked tear duct1 are most frequently seen in babies, they can occur at any age and have a variety of causes.
In most cases, blocked tear ducts resolve without medical intervention and do not cause any permanent eye problems. In some cases, however, a blocked tear duct will need medical treatment and may indicate a more serious problem, such as a tumor. As such, it is important to consult with one of our experienced Orange County ophthalmologists if you suffer from a blocked tear duct.
These symptoms can be caused by the blocked tear duct2 or may be a side effect an infection that has occurred due to the blockage.
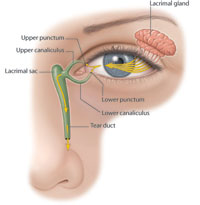
Tears are primarily produced by the lacrimal glands, which are located inside the upper eyelids over each eye. In a healthy eye, tears travel down from these glands over the surface of the eye and drain into tiny holes known as puncta, which are located in the corners of the upper and lower eyelids. From here, the tears move into the lacrimal sac located at either side of the nose where they then flow down a duct that drains into the nose. A blockage can occur anywhere within this complex and delicate drainage system. If this happens, tears will be unable to drain properly, resulting in watery, leaking eyes and increasing the risk of infection and inflammation.
A blockage within the tear drainage system can be caused by a variety of reasons and can happen at any age. Common causes include:
To diagnose a blocked tear duct, our Huntington Beach ophthalmologists conduct a thorough eye exam and use a few tests to determine how well the patient's tears are draining. During the appointment one or more of the following tests may be conducted to identify the cause and location of the blockage:
Tears serve an important purpose – they keep the eye moist and clean so that bacteria, viruses, and fungi do not infect the eye. When a blocked duct prevents the eyes from draining properly, recurrent infections are likely to occur. It is important to see one of our eye doctors if your eye is frequently infected, seems to be excessively watery, or if your vision is blurry. Dr. Wenjing Liu is an eyelid and tear duct specialist (also known as an Oculoplastic specialist) that can address all your concerns and treat your condition.
In treating a blocked tear duct, the goal is to remove the obstruction so that the tear drainage system begins to flow properly once again. Our eye doctors typically recommend a conservative approach to treat blocked tear ducts, as most cases will resolve spontaneously within a few months.
In newborns, blocked ducts usually resolve during the first few months of life. If they do not, our eye doctors may teach the parents how to perform a special massage technique designed to help the nasolacrimal duct open up. When the blocked duct occurs in children or adults as a result of injury, it is best to give it time, as the blockage may resolve after swelling decreases.
When time does not resolve the issue, the next step is to attempt one of the minimally invasive treatments available. Our eye surgeons are experienced with new techniques that can solve your condition without an intrusive surgery:
Surgery should only be performed if a less invasive treatment did not resolve the blocked tear duct. Dr. Wenjing Liu sees many patients each year with similar conditions and will prepare a personalized treatment plan for you to give you the best possible outcome.
Dacryocystorhinostomy, the surgical technique used to resolve blocked tear ducts, can be performed under general or local anesthesia. The goal of this surgery is to create a new passageway for tears to drain into the nose. The new passageway will bypass the nasolacrimal sac completely, as this is the most common site of persistent blockages that cannot be resolved through less invasive methods. Stents or tubes are used to hold the newly created passageways open while the body heals, which can take up to 3 months.
When performed by one of our skilled eye surgeons, dacryocystorhinostomy can be a very effective treatment for blocked ducts. Because the surgery addresses such a delicate and important facial structure, it is important that it is performed by an ophthalmologist or eye surgeon who is highly experienced at performing dacryocystorhinostomy, particularly an Oculoplastics specialist.
If you are suffering from a blocked tear duct, please contact Beach Eye Medical Group today. We serve all parts of Orange County! Click here to schedule an appointment or call us (714) 965-9696.
References
1 What Is a Blocked Tear Duct? Available: https://www.aao.org/eye-health/diseases/what-is-blocked-tear-duct
2 Blocked tear duct. Available: https://www.mayoclinic.org/diseases-conditions/blocked-tear-duct/symptoms-causes/syc-20351369
Beach eye medical is the best! The staff is very friendly and helpful. Dr D.McCluskey is the best!

Medically Reviewed by
Samir Shah, MD
Samir Shah, MD, MS, FACS, is a board-certified ophthalmologist specializing in custom laser cataract surgery and refractive lens exchange. A Johns Hopkins fellow and UCLA alumnus, he is nationally recognized as an expert in refractive cataract surgery. Recently, he was named the Top Doctor 2026 by the Orange County Medical Association and Orange Coast Magazine.