Age-related macular degeneration (AMD) is a deterioration or breakdown of the eye’s macula. The macula is a small area in the retina — the light-sensitive tissue lining the back of the eye. The macula is the part of the retina that is responsible for your central vision, allowing you to see fine details clearly.
Even though the macula makes up only a small part of the retina, it is much more sensitive to detail than the rest of the retina, called the peripheral retina. The macula is what allows you to thread a needle, read small print, and read street signs. The peripheral retina gives you side (or peripheral) vision.
If someone is standing off to one side of your vision, your peripheral retina helps you know that person is there by allowing you to see their general shape. It is your macula that allows you to recognize the details of the person’s face.
Many older people develop macular degeneration1 as part of the body’s natural aging process. There are different kinds of macular problems, but the most common is age-related macular degeneration2.
The retina is made up of many layers that work together to help you see clearly. AMD develops when a layer under the retina called the retinal pigment epithelium (RPE) is affected by deposits of tiny yellow or white pieces of fatty protein called drusen, or by other age-related changes.
With AMD, you may have blurriness, dark areas or distortion in your central vision, and perhaps permanent loss of your central vision. It usually does not affect your side, or peripheral vision. For example, with advanced AMD, you could see the outline of a clock, yet may not be able to see the hands of the clock to tell what time it is.
AMD alone almost never causes total blindness. People with more advanced cases of AMD continue to have useful vision using their side, or peripheral vision. In many cases, macular degeneration’s impact on your vision can be minimal.
When AMD does lead to loss of vision, it usually begins in just one eye, though it may affect the other eye later.
Many people are not aware that they have macular degeneration until they have a noticeable vision problem or until it is detected during an eye examination.
Most people who have AMD have the dry form. This condition is caused by aging and thinning of the tissues of the macula. Macular degeneration usually begins when tiny yellow or white pieces of fatty protein form under the retina. These deposits are called drusen. Eventually, the macula may become thinner and stop working properly. With dry AMD, vision loss is usually gradual.
People who develop dry AMD must carefully and constantly monitor their central vision. If you notice any changes in your vision, you should tell your ophthalmologist (Eye M.D.) right away, as the dry form can change into the more damaging form of AMD called wet (exudative) AMD.
If you have been diagnosed with dry AMD, you should use a chart called an Amsler grid every day to monitor your vision, as dry AMD can change into the more damaging wet form.
If you have been diagnosed with dry AMD, you should use a chart called an Amsler grid every day to monitor your vision, as dry AMD can change into the more damaging wet form.

The wet form of macular degeneration occurs in about 10 percent of all macular degeneration cases, but it can cause more damage to your central or detail vision than the dry form.Capillaries, or tiny blood vessels, extend into all tissues of the body, bringing in nutrients and carrying off waste products. Capillaries usually don’t increase in size or number, but if they do, it is called abnormal blood vessel growth. The longer these abnormal vessels leak or grow, the more risk you have of losing more of your detailed vision. Also, if abnormal blood vessel growth happens in one eye, there is a risk that it will occur in the other eye. The earlier that wet AMD is diagnosed, the better chance you have of preserving some or much of your central vision. That is why it is so important that you and your ophthalmologist monitor your vision in each eye carefully.
Wet AMD occurs when abnormal blood vessels begin to grow underneath the retina. This blood vessel growth is called choroidal neovascularization (CNV) because these vessels grow from the layer under the retina called the choroid. These new blood vessels may leak fluid or blood, blurring or distorting central vision. Vision loss from this form of AMD may be faster and more noticeable than that from dry AMD.

In its earliest stages, macular degeneration may cause the following symptoms:
Doctors and researchers don’t know the exact causes of AMD but it is clear that this disease is strongly associated with age, since AMD occurs as people grow older. One large study found that the risk of getting AMD jumps from about 2 percent of middle-aged people in their 50s to nearly 30 percent in people over age 75.
Our bodies constantly react with the oxygen in our environment. Over our lifetimes, as a result of this activity, our bodies produce tiny molecules called free radicals. These free radicals affect our cells, sometimes damaging them. This is called oxidative stress and is thought to play a major role in how AMD develops.
Heredity is another risk factor for AMD. People who have a close family member with the disease have a greater chance of developing AMD themselves.
Some studies have shown that inflammation (swelling of the body’s tissues) may play a role in AMD development. Inflammation is the way the body’s immune system fights off infection or other things it considers “invaders.” But an overactive immune system with its associated inflammation may be a risk factor for AMD.
Smoking and high blood pressure are associated with the wet form of AMD. Research also suggests there may be a link between being obese and having early or intermediate-stage AMD develop into advanced (wet) AMD.
Many older people develop macular degeneration as part of the body’s natural aging process. Approximately 1 in 3 Caucasians have genetic changes that make them more prone to damage from oxidative stress, when certain molecules affect our cells, which can lead to AMD.
Major risk factors for AMD are:
Another risk factor for developing AMD may include having abnormal cholesterol levels or having high blood pressure (called hypertension).

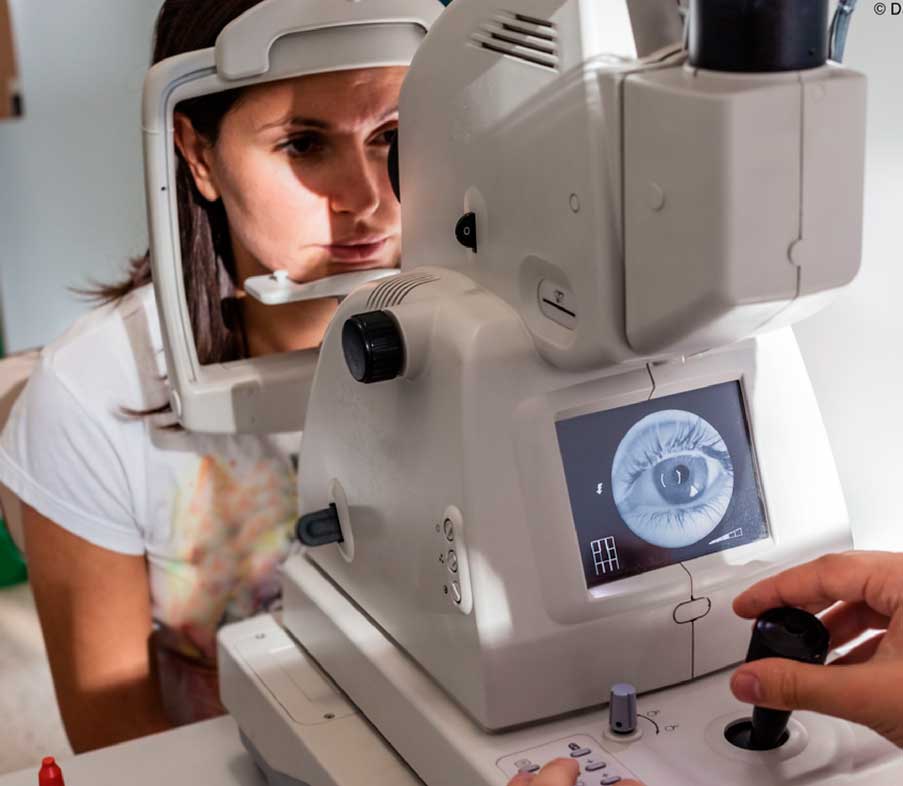
Many people do not realize they have a macular problem until they notice they have blurred or distorted vision. Regular eye examinations by an ophthalmologist may help to detect problems before you are even aware of them. Your ophthalmologist may see early stages of AMD during a comprehensive eye examination. A significant benefit of having your macular degeneration evaluation and follow up performed at Beach Eye Medical Group is that we have invested in the most advanced technology to monitor macular degeneration. We use the Cirrus HD OCT3 (Optical Coherence Tomography) from Carl Zeiss Meditec. With this instrument, we are able to detect subtle and small changes in your retinal health better than the human eye and better than ever before. Wherever you choose to go, make sure your eye care provider has invested in the best technology for you. Remember, early detection and treatment of macular degeneration may save your vision.
The American Academy of Ophthalmology recommends that adults with no signs or risk factors for eye disease get a baseline eye disease screening at age 40 — the time when early signs of disease and changes in vision may start to occur. Based on the results of the initial screening, an ophthalmologist will prescribe the necessary intervals for follow-up exams.
To check for macular degeneration, your eye doctor will dilate (widen) your pupils using eyedrops and examine your eyes with an ophthalmoscope, a device that allows him or her to see the retina and other areas at the back of the eye. If AMD is detected, your doctor may have you use an Amsler grid to check for wavy, blurry or dark areas in your vision.
The American Academy of Ophthalmology4 recommends that adults with no signs or risk factors for eye disease get a baseline eye disease screening at age 40 — the time when early signs of disease and changes in vision may start to occur. Based on the results of the initial screening, an ophthalmologist will prescribe the necessary intervals for follow-up exams.
To check for macular degeneration, your eye doctor will dilate (widen) your pupils using eyedrops and examine your eyes with an ophthalmoscope, a device that allows him or her to see the retina and other areas at the back of the eye. If AMD is detected, your doctor may have you use an Amsler grid to check for wavy, blurry or dark areas in your vision.

Vision Rehabilitation
Vision rehabilitation can help people with low vision compensate for vision loss. People with low vision can learn new strategies to accomplish daily activities. These skills, including mastering new techniques and devices, help people with advanced vision loss regain their confidence and live independently.How much rehabilitation is needed depends on your vision loss and what you want to be able to do. A team approach is often best and may involve some or all of the following professionals: ophthalmologist, low-vision specialist, occupational therapist, rehabilitation teacher, orientation and mobility specialist, social worker and counselor.This rehabilitation process can be a challenging and frustrating period of adjustment — one that requires patience, practice, motivation and the support of your doctor, low-vision specialist, family and friends. The rewards, however, can be great.
There are many devices specifically designed to help people with low vision function better. Different devices are available for different tasks. A trained professional can help you understand which device is best for accomplishing your particular needs. Training and practice are also important in order to become skilled at using any device.
Optical low-vision devices use lenses to magnify objects, making them easier to see. The lens strength will depend on your vision and the size of the object or print to be seen.
There are numerous low vision aids, devices, and techniques to help make everyday activities easier. They include:
Good lighting and glare control are very important for people with low vision. A bright light should always be used when reading and its location should be adjusted for the greatest visibility without glare.
Stronger light bulbs in darkly lit areas can make tasks like cooking, dressing, and walking up and down stairs easier. Wearing a hat with a wide brim or tinted wraparound sunglasses can shield your eyes from dazzling and annoying overhead lights or sunlight.
References
1 Age-Related Macular Degeneration (AMD). Available: https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/age-related-macular-degeneration
2 Age-Related Macular Degeneration. Available: https://www.webmd.com/eye-health/macular-degeneration/age-related-macular-degeneration-overview
3 Identifying subtle changes in pathology ZEISS CIRRUS HD-OCT. Available: https://www.zeiss.com/meditec/en/products/optical-coherence-tomography-devices.html
4 What Is Macular Degeneration? Available: https://www.aao.org/eye-health/diseases/amd-macular-degeneration
This place is great. I got an appointment on short notice. The facility is nicely decorated. All of the staff was friendly and professional. Dr. Shaw is down to earth and friendly.
THANK YOU!!!!!!!!!

Medically Reviewed by
Samir Shah, MD
Samir Shah, MD, MS, FACS, is a board-certified ophthalmologist specializing in custom laser cataract surgery and refractive lens exchange. A Johns Hopkins fellow and UCLA alumnus, he is nationally recognized as an expert in refractive cataract surgery. Recently, he was named the Top Doctor 2026 by the Orange County Medical Association and Orange Coast Magazine.